Monitor Your Chiropractic Practice Health at a Glance
Watch Your Chiropractic Practice Health and Get Back To Your Patients Faster Control your Chiropractic Practice Health! Chiropractic Practices rely on separate reports to understand where they are as a practice and a business. Separate reports require comparison and compilation in Excel or other spreadsheets to stack data and notice a trend over time. Comparison of rows of numbers is difficult without graphics to show trends. Imagine never pulling numbers out of reports to compare where you are and where your business is going. Imagine having a tool that enables you to track your daily business goals at a glance. Imagine the time savings that you can now spend with your patients. Well, imagine no more. The tool is called The Genesis Chiropractic Practice Health Monitor and you can learn about it in this 15 minute webinar.
Is Your Chiropractic Practice Ready for ICD-10?

In this webinar you will learn how to prepare your Chiropractic Practice for ICD-10. ICD-10 codes are unique with a basic five part structure, and there are add-ons. In this case, secondary or supplementary diagnosis codes are required to complete the process. This webinar will cover how to verify if all of your claims are using the correct ICD-10 codes. See the ICD-9 to ICD-10 transition and how easy it is to use.
Audit Proof Your Chiropractic Practice

An Audit Proof Chiropractic Practice is possible! Learn how to audit proof your Chiropractic Practice. Detect your audit risk areas at a glance. Improve your billing compliance by reducing unsigned notes and unbilled visits.
Seal Your Chiropractic Revenue Leaks

Learn how to track your Chiropractic Billing Performance and it’s impact on your office workflow, billing workflow and your billing results. The big secret is the Genesis Billing Stats Report. Read the transcript: Jess: Hi, my name is Jess, and welcome to today’s webinar on tracking revenue for your practice. Conducting today’s webinar are Kathy Casbarro, the head of our SWAT team who has 30 years of experience in Practice Management, and Jason Barnes, our Chief Operating Officer who is responsible for the billing performance for 500 practices. Welcome, Jason and Kathy. Jason: Hello, thank you for having us. And we’re really excited about this whole series of webinars that we get to put on. More importantly, Jess, is that we’re more excited about helping the entire chiropractic profession. When it comes to running a practice these days, we understand how many balls that a practice owner has to juggle. And for those of you on the phone today, we get to personally hear those stories. Kathy, who I’ve worked with now for four years, and I get to interact with practice owners on a regular basis, talk to them about their frustrations, about their successes, the things that really drive them. And the fact that the mission that the entire chiropractic community shares for changing healthcare is really the main driver, makes the talk of money seem sometimes misplaced. But we know that without a solid financial backing, that mission will never be realized. So, we want to start from that perspective today and really make sure that by talking about money, we can help achieve that dream, that mission, that we share with chiropractors. And Jess, let’s get to the next slide here. We wanna start out by helping practice owners understand what we’re trying to do. As an organization, we help practices in a number of different ways, scheduling, billing, documentation, and practice management. But today, we wanna focus on the revenue portion of that. We can’t break out just the billing without talking about your scheduling process, the intake process. When you’re talking about sealing revenue leaks, looking at the entire practice as a whole has to be part of the approach. And Kathy and I, working together over the last few years, know that when you’re talking about office workflow or billing workflow, they’re really the same conversation most of the time. We separate them in this context to help people understand that when you’re looking at lower collections than what you’re expecting, that can be a frustration that can be scary because we know practices that can’t last for more than just a few months without writing that chip. So, today, we wanna focus on understanding where in your process their breakdown occurred so that we can specifically identify it and then figure out a plan to solve it. But identifying it is without a doubt the first key. So, knowing where you’re reimbursement gets stuck, as Kathy and I have worked together, Kathy, when you talk to practices, what’s the biggest frustration you get from practice owners when they’re not realizing the collections that they thought they would have? Kathy: It’s when they’re not, you know, they can’t continue to treat their patients the way they want to, you know, being able to continue with their mission, so the frustration is that they need to bring in the money in order to continue that mission to help every patient that they have in their practice and, you know, that can be a problem for them. Jason: Yeah. So, when that frustration happens, maybe their heart is not into treating the patients the way they wanted to because they’re worried about whether or not they can keep the doors open. We’ve actually had those conversations. I don’t wanna be overdramatic about it, Kathy, but it’s unfortunate. We’ve seen people forced to sell their practices and move backwards back to the role of associate while they figure out how to attack the problem again. We wanna help people avoid that. We wanna see the chiropractic profession really explode, and I think we’re in a good position to help there. So, keep in mind, just kind of recap as I go through this, coming up with a process that’s repeatable for your office workflow, your intake process, is the only way that sealing your revenue approach that we came up with works. If you don’t have a set process, then there’s really difficulty in trying to diagnose it. But you have to make sure that you understand the connectors you’re looking at. So, some of the examples that we’re talking about today is CPT codes. Am I in or out of network? Am I gonna get paid a certain amount? Do I know what that amount is supposed to be? We need to ask those questions and then be able to track the data across many months. And we deal with the smaller, you know, one chiropractor, part-time front office practices, and we got 10 locations, I’ve got 22 chiropractors, 6 physical therapists, I’ve got weight loss, and I need to make sure all of that is running together. So, the difference between them is actually really, really small. Because the intake process, the data collection process that you have to follow is nearly identical. But now we have to track whether or not the breaking points are the same. And in our experience, they’ve been really, really similar. So, Jess, can you hit the next one for us? We know that you can’t operate and fix the problem at the same time. So, the amount of time that it takes you to come up with a root cause analysis of where your practice went wrong is critical. It’s critical to you enjoying a family life or work outside of your office. Kathy, with some of the more complex problems, how much time does it take to actually figure out where the process is broken
PQRS – How 4 letters affect your Practice
Unless you are billing the right set of PQRS codes on 50% of your qualifying visits, then you will lose 2% of your allowed reimbursement. Learn about the changes that this reporting system brings to your practice. Understand how this reporting system affects your reimbursements plus know how and when to use these codes. Read the transcript: Jess: All right. Thank you everyone for joining us today for our webinar on PQRS. Today’s instructors are Kathleen Casbarro and David Alben [SP]. Kathleen is the head of our Billing SWAT department here at Vericle and she has 30 years of experience in this industry. And she is a certified coder. David Alben helps practices achieve and maintain a culture of compliance. He is alsot he also assists healthcare attorneys in defending their clients who have been audited or are subject to prepayment review. So he has his finger on Medicare’s expectations and when it comes to medical documentation. So welcome, Kathleen and David. Kathleen: Thanks so much Jess [SP], really appreciate that. So welcome everybody. I was told about some of the people that registered, and I’ve seen some familiar names. So I’m really glad you’re able to spend a half an hour with us today. So our focus today is going to be on PQRS. We have a single learning objective for today and that is really understanding the PQRS requirements and, you know, Medicare’s rules and the cost of PQRS to your practice. So there could be several of you on the phone that say to yourself, “Well, what is PQRS? What does it stand for? You know, why do I have to go ahead and report another set of claims to the insurance company? I mean, it just sounds like there’s a lot to juggle.” What we wanna talk to you about is, first off, is what is PQRS? So PQRS stands for the Physician Quality Reporting System. It was actually renamed from the Physician Quality of Reporting Initiative. So it used to be PQRI, if anybody familiar with that, and now it’s PQRS. They changed the acronym. The reason why we have PQRS is CMS is wants to make sure that, you know, the patient is getting the right care, that you’re providing the quality of care to your patient. And they wanna make sure that the patients are getting the right care at the right time. That’s what this system is actually built. It was actually built for reporting outcomes. The other thing that they wanna do, too, and Dave is really here to talk about that, I brought Dave on really for the auditing part of this, is, you know, quantifying how they’re meeting the particular quality measure. And Dave, how do you suggest the practice does that? David: So I think it’s important to, first up, really understand what Medicare is looking for, which we’re talking about today. And the other aspect of it is that you pretty much have to patrol your own house, keep it in order, auditing your own claims to make sure that you’re meeting the standards and the number of claims that you need to report on on a…at least a quarterly basis, maybe a little more frequently at the beginning and that everyone on your team understands the significance of this, and why it’s important to the practice. Kathleen: Right, I agree. So the feedback that CMS is getting from this is they’re gonna compare your performance with other peers in your same specialty. And really, the overall goal here is to make changes to payment structures and implement new rules. So, you know, a lot of times you put things on the back burner but, you know, we’re gonna get into later on why really it’s not a good time to do that. We talked about PQRS and what it is and really what it stands for. So, you know, what’s the problem? Why is PQRS a problem? Well, PQRS is a problem because what’s gonna happen is that right now for 2013, the requirements have actually changed. For 2013, you had to report on 20% of your eligible patients within the year and only report on three measures, okay? If you didn’t do that, you’re gonna be penalized by Medicare in 2015 and that’s based on your Medicare allowable. By the way, nobody knows on this call what the Medicare allowable is going to be in 2015. I wish I had a crystal ball for you but I don’t. So for 2014, the rules have changed. So now we go from 20% of your eligible patients now having to report on 50% of your eligible patients. I know most of you out there are going, “Well, what’s an eligible patient? Is that all my Medicare patients?” And we’re gonna get into that, and, you know, nine reporting measures. “Well, what if I don’t have nine reporting measures? What if I only have three? Will I still be penalized?” And we’re gonna get into that as well. But what I’m trying to show here is that you’re trying to juggle a lot of things right now and things are now changing in the industry. Fifty percent of your eligible patients, nine reporting measures, if you don’t report for PQRS in 2014, you’ll have a 2% reduction on your Medicare allowables for 2016, ’17, ’18, ’19, ’20, and so on until they stop. So just remember that. It’s 2016 onwards, not just 2016. So that’s why this is such a huge problem, because this is not going to affect one year. We kinda then have to talk to why is the problem important? The problem is hugely important for a specific reason. Anytime CMS implements something, and they want you to be part of something because they want to make an effect in your industry. So I represented this by a fish bowl effect. On the left-hand side, we have a couple of fish just swimming around,
The Secret to Understanding Chiropractic Practice Cashflow

Obviously, Cashflow will help your Practice grow! On Cashflow: Practice owners and staff regularly have questions about where their payments are, how they can see which insurance companies are helping them, and/or which patients are struggling to pay their bills. Fortunately, with a single report, practices can now periodically review where their payments are and how well their office is functioning, while comparing the metrics that are most important to their success. Watch this free webinar to learn more.
Own the Phone with Spencer Peller

Spencer Peller is the Co-Founder and CEO of YesTrak and Founder and CEO of MyDoctorCalls. He is also the author of the new book Own the Phone! Today’s training is all about your telephone! If you’re a business owner, you know how important your telephones really are. This training will help you understand every aspect of answering the phone. It’s also a great training for your staff, so make sure you send this link to them and tell them to watch it. Click the interview below to get started… For more information about YesTrak: Visit: www.YesTrak.com Call: (800) 620-5877 Send email to info@yestrak.com
The Secret to Better Practice Management Decisions

Learn how to use metrics for better decision making! Metrics are what you need. When it comes to managing your practice, it’s often difficult to make informed, timely decisions without data. That’s because practice owners are frequently unsure of which performance indicators they should measure, or even how to get started. Or, they ignore the data and operate on instinct. Analytics, however, take the guesswork out of practice management, while simplifying the data so it can be easily understood. These tools provide increased efficiency and effectiveness, for improved decision-making ability.
How to Build a Huge Chiropractic Practice with Dr. Stephen Franson!

Dr. Stephen Franson has not only built a huge, wellness based Chiropractic practice, but he’s also helped dozens of Chiropractors to do the same thing. He has studied the process of building successful practices and teaches it to Chiropractors from around the globe. Dr. Franson is the founder of The Remarkable Practice where he shares his research and strategies. In this interview he will tell you all about the lifecycle of his practice (a 1,000 visit per week office), and how he closed the “side doors” on his office and converts most of his corrective care patients to longterm family wellness plans. Check out this quick video interview below, and then leave us a comment! For more info on The Remarkable Practice Click Here
Revenue | Committing to a Software Solution

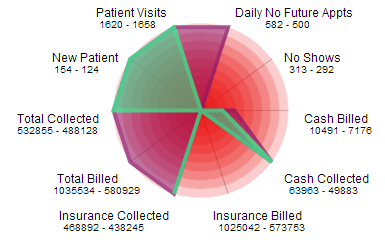
Much Ado About Data Committing to a Software Solution Can Dr. Ben move past being overwhelmed by data and commit to Genesis? As he made his way into work on Monday, Ben was preparing himself to take the next step in his Genesis journey. He knew that the software was going to help in innumerable ways, from records management, to tracking insurance payments, to helping to get patients reinvested in their own care plans. But with reports come data – a TON of data – and what on earth were he and Luisa going to do with all of those numbers? “Good morning Luisa,” Ben said as he entered the office. “Hello Dr. Ben – how was your weekend?” asked Luisa. “It was great,” Ben answered. “Carmen and I tried out the new downtown Indian buffet. It’s really good – and I even have leftovers to enjoy for lunch today!” “Hopefully Jonathan found something he liked to eat, too,” said Luisa. She stopped for a minute, then continued, “So… have you given any thought to moving forward on Genesis?” Ben sighed. It was going to be difficult to put this off for any longer. “I know, I know, we shouldn’t wait any longer,” he said. “Before we get started, I’m going to call our coach, Charlie, and ask her a few questions.” “Let me know if there’s anything I can do,” said Luisa. Ben placed his lunch in the refrigerator and then went into his office, closing the door. He stared at the phone for a minute and then laughed at himself. Boy, change can really be hard, he thought. He picked up the phone and, within a minute, he was connected with his Genesis coach, Charlie. “How are things going, Dr. Ben?” Charlie asked. “Well, we’re doing fine but … I have to admit, we understand that this software is going to help us manage the office more professionally and efficiently but we’re having trouble taking that last big step and rolling it out,” Ben admitted. “Oh, you’re not alone,” Charlie said. “Ask me anything – we’re here to help!” “I guess we’re overwhelmed by all the data,” said Ben. “Neither Luisa nor I are number crunchers, and the reports can get so complex. How can we be sure that this is going to help us, rather than adding to our already busy workdays?” “One of the wonderful things about the billing stats report is that it will help you to create consistent, repeatable processes for collecting patient information and assessing billing performance,” Charlie said. “It might be daunting looking at the possibilities from the outside in, but once you’ve got things set up, it will actually help you to get a handle on your office cash flow and more easily identify where – and why – things are being held up in the reimbursements pipeline.” He continued, “Have you ever looked at your revenue stream over a period of a few months and seen a decline, and panicked? With the billing stats report, instead of trying to go patient by patient, week by week, month by month, and guess what the problems are, you can actually run reports with up to 45 different parameters and pinpoint where exactly in the process things are breaking.” “I don’t see how that is possible,” protested Ben. “Let me put it this way: you can run a 60-day report and get a breakdown of the status of each claim,” said Charlie. “If the claim is not at the insurance company, then you’ll be able to figure out if you’ve got an intake problem, if your claims are going out in a timely fashion, or if there are issues with the information you’re sending out with the claim. You can also look at which CPT codes are getting paid or underpaid. With the power of accurate statistics, you can have the right conversations with front desk staff, your office manager and billers.” “What’s also great is that with the radar chart, you can set parameters for your practice,” Charlie continued. “If you get to a point where everything is within the parameters you’ve set, then you will render the billing stats report unnecessary. That’s a terrific thing about Genesis – we help you achieve best practices in your office management so that you can be in control of your practice and focus more on your patients.” “That’s exactly what we want,” said Ben. “I don’t know anyone who went into medicine so that they could spend most of their day staring at a computer screen!” “But do you want to hear the most wonderful thing of all about Genesis?” Charlie asked. “Of course,” said Ben. “Whenever you have a question, a concern or simply want to talk through some numbers that don’t seem to make sense, you can call me,” Charlie said. “We are committed to being here when you need us.” “Well, that is the most wonderful thing I’ve heard all day!” laughed Ben. “I can’t thank you enough for your time today.” After a few more minutes of small talk, Ben emerged from his office and walked toward Luisa, who knew just by looking at him that change was afoot. “That must have been some phone call,” said Luisa. “It was,” smiled Ben. “I think we’re ready to begin our Genesis adventure – together!” Is Dr. Ben ready for launch? Disclaimer: For HIPAA compliance, all characters appearing in this post are fictitious. Any resemblance to actual persons or actual events is purely coincidental.

