Mental Health Practice Statistics, 2026 State of the Industry
The Numbers Shaping Behavioral Health Practices We analyzed mental health practice statistics across workforce trends, telehealth adoption, reimbursement benchmarks, and market growth indicators. This report brings together federal workforce projections, market research, and insurance claims data to help behavioral health leaders understand the numbers shaping practice performance and long-term strategy. The latest mental health practice statistics reveal a market defined by strong demand and persistent operational pressure. Patient need is rising, provider shortages are worsening, telehealth has become a permanent part of care delivery, and reimbursement continues to vary widely by payer. For practice owners and administrators, these trends are not just market signals. They directly affect staffing, scheduling, revenue, and growth planning. Mental health practice statistics on the workforce shortage Among the most urgent mental health practice statistics in 2026 is the scale of the behavioral health workforce gap. The United States continues to face severe shortages across counseling, psychiatry, psychology, addiction treatment, and social work. By 2038, the projected gap between supply and demand is expected to remain substantial across multiple provider types. Projected behavioral health provider shortages, 2038 Provider Type Projected Shortage (FTEs) Percent Adequacy Mental Health Counselors -99,780 to -203,690 38% to 55% Psychologists -99,840 to -152,520 37% to 48% Addiction Counselors -77,050 to -123,270 21% to 30% Adult Psychiatrists -36,780 to -86,430 30% to 50% Marriage & Family Therapists -33,840 to -63,540 45% to 60% Mental Health Social Workers -17,030 to -62,060 62% to 85% These mental health practice statistics also show how widespread the access issue has become: 40% of the U.S. population, about 137 million people, lives in a Mental Health Professional Shortage Area 48% of adults with mental illness did not receive treatment in 2024 69% of rural counties lack psychiatric nurse practitioners 6 in 10 psychologists were not accepting new patients as of 2025 This workforce crisis creates a difficult operating environment, but it also creates opportunity for practices with the systems and capacity to serve unmet demand. Sources Health Resources and Services Administration, State of the Behavioral Health Workforce, 2025. Mental health practice statistics on telehealth adoption Telehealth remains one of the most important mental health practice statistics categories because behavioral health continues to lead all specialties in virtual care utilization. What began as a pandemic-era necessity is now a lasting part of mental health service delivery. Telehealth utilization in behavioral health Service Category 2020 Peak 2023 Stabilized Rate Share of Telehealth Visits Top Diagnoses Behavioral Health Providers 35 per 1,000/month 35 per 1,000/month 58% Anxiety, depression, PTSD Primary Care Providers 69 per 1,000/month 15 per 1,000/month 18% Chronic disease management All Mental Health Related N/A N/A 58%, up from 47% in 2020 Anxiety and mood disorders Additional mental health practice statistics reinforce the permanence of this shift: Mental health services represented 58% of all telehealth visits in 2023 Rural Medicaid patients made up 40% of rural telehealth visits Urban commercially insured patients made up 42% of urban telehealth visits These mental health practice statistics make one point especially clear: telehealth is now a structural part of behavioral health access, retention, and growth. Sources Center for Improving Value in Health Care, New Telehealth Analysis Shows Sustained Demand for Mental and Behavioral Health Services. Mental health practice statistics on reimbursement rates Reimbursement remains one of the most consequential areas for practice performance. The latest mental health practice statistics show major variation by payer type, with Medicare and some commercial plans generally reimbursing at stronger levels than Medicaid and managed care. Mental health reimbursement ranges by payer type, 2026 Payer Category CPT 90834 CPT 90837 Relative Payment Billing Complexity Medicare $113.90 $167.00 High Moderate to High BCBS Networks $110 to $140 $160 to $210 High Moderate Anthem / Aetna / Cigna $90 to $120 $130 to $180 Above Average Low to Moderate UnitedHealthcare / Optum $85 to $110 $125 to $165 Average Moderate Medicaid $60 to $85 $90 to $125 Below Average High Medicaid Managed Care $55 to $75 $80 to $110 Low Very High Other key mental health practice statistics in reimbursement include: Medicare increased CPT 90834 reimbursement from $104.16 in 2025 to $113.90 in 2026 Only 46% of psychiatrists accepted Medicaid from new patients as of 2017 Commercial insurance participation is still limited by admin burden, delayed payment cycles, and lower reimbursement relative to private pay High-cost metro areas can command premium commercial rates These reimbursement trends highlight why payer mix remains a critical growth decision for mental health practices. Sources Health Resources and Services Administration, State of the Behavioral Health Workforce, 2025. TheraThink, Mental Health Reimbursement Rates by Insurance Company, 2026. What these mental health practice statistics mean for practice leaders Taken together, these mental health practice statistics show a behavioral health market with clear growth potential and equally clear operational challenges. Demand is rising faster than provider supply. Telehealth has become essential. Reimbursement varies significantly by payer. Administrative burden continues to influence profitability and provider participation. For practice leaders, the takeaway is simple: growth in 2026 depends not only on clinical demand, but on the ability to manage operations efficiently. Practices that streamline scheduling, documentation, telehealth, billing, and reimbursement workflows will be better positioned to capture demand and support long-term performance. About This Report This in-depth report was prepared for ClinicMind. Sources Health Resources and Services Administration, State of the Behavioral Health Workforce, 2025. Precedence Research, Behavioral and Mental Health Software Market Size to Reach USD 30.62 Billion by 2034. Center for Improving Value in Health Care, New Telehealth Analysis Shows Sustained Demand for Mental and Behavioral Health Services. TheraThink, Mental Health Reimbursement Rates by Insurance Company, 2026. Lawrence, Evans & Co. LLC, Behavioral Health Market Update Q1 2025.
Why Messaging Breaks in Family-Based Clinics (And How to Fix It)
In many healthcare practices—especially chiropractic, pediatric, behavioral health, and family medicine clinics—communication doesn’t happen at the individual level. It happens at the family level. A single phone number often represents multiple patients. Parents manage appointments. Caregivers coordinate care. Guardians stay involved in behavioral health treatment. Yet most patient communication systems are built for individuals—not families. This disconnect leads to fragmented messaging, slower response times, and poor patient experiences. In this guide, we’ll break down: Why healthcare messaging systems fail family-based clinics The operational impact of fragmented communication How centralized communication platforms like PatientHub solve it What Is Family-Based Patient Communication? Family-based communication in healthcare refers to managing patient interactions through a shared contact (such as a parent, guardian, or caregiver), rather than treating each patient as a completely separate communication channel. This is especially common in: Pediatric clinics Chiropractic practices Behavioral health clinics (where caregivers are often involved in care coordination) Family medicine practices This model is common in patient communication workflows across chiropractic, pediatric, and behavioral health practices, where one contact manages multiple patient interactions. The Core Problem: Healthcare Messaging Systems Built for Individuals Most patient communication software platforms are structured around individual patient records Each patient has: Their own chart Their own appointments Their own medical history That makes sense clinically. But communication doesn’t follow that same structure. When one phone number is tied to multiple patients, systems often: Split conversations across multiple profiles Store messages under different patient records Fragment conversation history This creates a disconnect between real-world workflows and system design. What Fragmented Messaging Looks Like in Practice When a parent or caregiver messages your clinic: Staff must search across multiple contact records Conversation history appears incomplete or scattered It’s unclear which patient the message refers to This is even more complex in behavioral health, where: Multiple family members may be involved Privacy and clarity are critical Context matters for every interaction As a result, front desk teams spend extra time: Verifying context Switching between records Reconstructing conversations The Hidden Cost of Fragmented Healthcare Messaging What seems like a small inconvenience quickly compounds into real operational issues. 1. Healthcare Messaging Inefficiencies Staff must gather context before replying. 2. Increased Risk of Errors Messages can be tied to the wrong patient or miss key details. 3. Higher Training Burden New staff must learn workarounds instead of intuitive workflows. 4. Onboarding Friction Fragmented systems are harder to explain and adopt. 5. Patient Communication Breakdown Patients and families expect seamless communication—but often get inconsistency. These communication breakdowns don’t just slow your team down—they directly impact revenue through missed appointments, lost follow-ups, and patient churn. If you want to quantify how much these inefficiencies are costing your clinic, you can use a patient engagement ROI calculator to estimate the financial impact of poor communication. Why Traditional Patient Communication Software Falls Short This is a limitation of legacy healthcare communication platforms, not your staff or workflows. Most systems are designed to manage communication at the patient level, while real-world communication happens at the contact level—especially in family and behavioral health settings. That mismatch forces clinics to adapt their workflows around software limitations. What Modern Patient Communication Should Look Like To fix this, communication systems need to reflect how clinics actually interact with patients and families. A modern centralized patient communication platform should include: Centralized Communication All messages from a shared phone number live in a single conversation thread. Primary Contact Structure A designated contact (e.g., parent or caregiver) becomes the communication anchor. Individual Patient Integrity Each patient still maintains: Separate clinical records Accurate appointment history Individual care data This ensures clarity, efficiency, and compliance—especially important in behavioral health environments. The Shift to Centralized, Family-Based Communication Modern clinics—including chiropractic, pediatric, and behavioral health practices—require a hybrid model: Shared communication at the contact level Individual records at the patient level When communication is centralized, staff can: Instantly understand who is messaging View full conversation history in one place Respond faster and more accurately Platforms that unify messaging—combining SMS, email, and other channels into one centralized hub—help eliminate fragmentation and streamline workflows. Why Centralized Communication Drives Clinic Growth Improving your patient communication system directly impacts: Front desk efficiency Staff confidence Onboarding speed Patient and family satisfaction In behavioral health practices especially, clear and consistent communication builds trust and continuity of care. Small inefficiencies in communication don’t stay small—they scale with your clinic. How PatientHub Solves Family-Based Communication PatientHub is a centralized patient communication platform built for modern healthcare practices, including behavioral health, chiropractic, and multi-provider clinics. Two-way messaging in a centralized platform Unified communication across SMS, email, and more Conversation tracking in one place Automation tools that reduce manual follow-ups This allows clinics to manage communication more efficiently while maintaining accurate patient records. Conclusion Family-based communication isn’t an edge case—it’s the norm across many healthcare specialties, including behavioral health. Systems that fail to support it create unnecessary friction for both staff and patients. By shifting to a centralized, contact-based communication model, clinics can: Eliminate confusion Reduce operational overhead Improve response times Deliver a better patient experience
Chiropractic Industry Statistics – 2026
The chiropractic profession is one of the largest non-physician healthcare workforces in the United States. This page compiles employment, compensation, geographic, and patient data from the Bureau of Labor Statistics, the American Chiropractic Association, and industry analysis sources. Key Takeaways Approximately 70,000 chiropractors are currently licensed in the United States, with ~41,480 employed in clinical settings as of 2023 (BLS). Employment is projected to grow 10% from 2023 to 2033, adding roughly 6,100 new jobs. The median annual salary for chiropractors is $76,530. The top 10% earn over $142,580 per year. Chiropractors treat more than 35 million Americans annually (ACA). Spinal manipulation accounts for approximately 45.9% of chiropractic market revenue (industry analysis). Back pain remains the leading diagnosis, affecting more than 70% of the population at some point in their lives. North America holds approximately 42.23% of the global chiropractic market as of 2024 (industry analysis). Chiropractic Industry Workforce & Employment Data As of 2023, approximately 70,000 chiropractors are licensed in the United States, with roughly 41,480 employed in direct clinical practice according to BLS survey data. An additional 3,000 work in academic and management roles, and approximately 11,000 chiropractic students are currently enrolled across 19 nationally accredited doctoral programs. The profession graduates approximately 2,800 new practitioners annually. Employment is projected to grow at a rate of 10% from 2023 to 2033 (faster than the average for all occupations), driven by an aging population and increasing demand for non-drug pain management. Metric Data Source Licensed chiropractors (U.S.) ~70,000 ACA Employed in clinical practice (2023) 41,480 BLS OEWS Working in academic/management roles ~3,000 ACA Current chiropractic students (U.S.) ~11,000 ACA New practitioners entering workforce annually ~2,800 ACA Accredited doctoral programs (U.S., Canada, Puerto Rico) 19 ACA Projected employment by 2033 ~61,200 (clinical) Industry analysis Projected employment growth (2023–2033) 10% (+6,100 jobs) Industry analysis Note: BLS employment figures reflect wage-and-salary workers only. The full licensed workforce figure (~70,000) from the ACA includes self-employed practitioners, which represents a significant portion of the profession. Chiropractic Industry Salary & Compensation Benchmarks Chiropractor compensation varies considerably by setting, geography, and patient volume. The BLS reports a median annual wage of $76,530 as of May 2023, with the top 10% earning more than $142,580. The highest-paying settings tend to be hospitals and employment services firms, not private practice. National Wage Distribution Percentile Hourly Wage Annual Wage 10th percentile $19.21 $39,960 25th percentile $27.88 $57,980 50th percentile (Median) $36.79 $76,530 75th percentile $49.00 $101,930 90th percentile $68.55 $142,580 Mean annual wage $43.15/hr $89,760 Wages by Industry Setting Industry Setting Annual Mean Wage Notes General Medical & Surgical Hospitals $125,870 Highest-paying setting Employment Services $105,930 Contract/per diem roles Outpatient Care Centers $101,660 Multi-provider settings Offices of Other Health Practitioners $89,130 Majority of employment (36,960 DCs) Offices of Physicians $84,080 Integrated care settings Top-Paying Metro Areas Metro Area Annual Mean Wage Anchorage, AK $147,240 Reno, NV $134,410 Riverside-San Bernardino-Ontario, CA $122,870 Killeen-Temple, TX $122,260 Rockford, IL $120,570 Geographic Distribution & Market Concentration Chiropractic employment is concentrated in high-population states, but the highest concentration relative to local workforce size is found in the upper Midwest, particularly North Dakota, Nebraska, and Iowa. The states with the most total chiropractors (Texas, California, Florida, New York, Illinois) reflect overall population, not per-capita demand. States with Highest Total Employment State Total Employment Jobs per 1,000 Workers Annual Mean Wage Texas 3,420 0.25 $94,040 California 3,410 0.19 N/A (not released) Florida 3,360 0.35 $85,380 New York 3,330 0.35 $93,540 Illinois 2,590 0.43 $69,480 States with Highest Concentration (Location Quotient) Location quotient (LQ) measures how concentrated an occupation is in a state relative to the national average. An LQ above 1.0 means the state has a higher-than-average share of chiropractors per worker. State Employment Location Quotient Annual Mean Wage North Dakota 260 2.25 $80,200 Nebraska 600 2.21 $72,260 Iowa 930 2.21 $69,650 Wyoming 140 1.92 $62,530 South Dakota 220 1.79 $87,450 Regional & Market Segmentation The following data is drawn from industry analysis of the U.S. chiropractic market. Segment Data Point Context Suburban market share (U.S.) ~62% of total revenue Highest population density + awareness Rural CAGR ~27.2% Fastest-growing segment; expanding healthcare access North America global market share ~42.23% (2024) Largest share globally Asia-Pacific projected CAGR (through 2030) ~13.96% Driven by health awareness and urbanization Franchise segment projected CAGR ~28.5% Standardized delivery driving accessibility Chiropractic Patient Volume & Treatment Breakdown More than 35 million Americans, adults and children, visit a chiropractor each year (ACA). The profession is most frequently consulted for musculoskeletal conditions, particularly back and neck pain. Three in four patients (77%) describe chiropractic care as very effective. Treatment Type by Revenue Share (Industry Analysis) Treatment Category Market Revenue Share Primary Conditions Addressed Spinal manipulation ~45.9% Back pain, neck pain, headaches Pain management services (all types) ~53.2% Chronic and acute pain Soft tissue therapy & exercises Included in above Musculoskeletal recovery, long-term function Leading Diagnoses Condition Market Share / Prevalence Back pain ~24.3% of global market share; affects 70%+ of population Neck pain High prevalence; 10–15% chronic/recurring Headaches/fibromyalgia 10–20% of patient visits combined Neuromusculoskeletal (NMS) diagnoses Majority of all chiropractic encounters Patient Demographics Age Group Revenue Contribution Common Drivers Adults 18–64 ~62.34% of market revenue Work injuries, posture, musculoskeletal discomfort Adults 60+ (geriatric) ~52.7% of patients treated Age-related degeneration, mobility, pain management Children & adolescents 10–15% of chiropractic visits Posture, birth trauma, sports injuries Patient Satisfaction Data Metric Finding Source Rate care as ‘very effective’ 77% of chiropractic patients ACA consumer survey Chiropractic vs. other back pain treatments Outperforms prescription medication, deep-tissue massage, yoga, pilates, and OTC medication in consumer surveys ACA Highest-rated provider for low back pain Above physical therapists, specialist MDs, and primary care MDs ACA Pain reduction with manual-thrust manipulation 94% of recipients experienced ≥30% reduction in pain vs. 54% for medical care recipients ACA clinical trial Chiropractic Within the Broader Healthcare System Chiropractic care is recognized by major clinical and federal healthcare
What Practices Should Know About EHR Data Security in 2026
By Erez Lirov, Chief Technology Officer, ClinicMind Healthcare practices are operating in an increasingly complex digital environment. Electronic Health Records (EHRs), telehealth systems, clearinghouses, billing integrations, and cloud-hosted platforms have dramatically improved efficiency and access to care. At the same time, they have expanded the cybersecurity risk landscape in ways that demand immediate attention and strategic investment. As we move into 2026, EHR data security is no longer simply an IT function. It is a core operational and leadership responsibility. At ClinicMind, we work with practices every day that are navigating these challenges, and we’ve come to recognize that the organizations thriving today are those treating security as a competitive advantage, not a compliance burden. The Escalation of Cyber Threats in Healthcare Healthcare remains one of the most targeted industries for cybercrime. In 2025, ransomware attacks against healthcare organizations continued at record levels, disrupting hospitals, specialty clinics, and outpatient networks nationwide. Threat actors increasingly leverage ransomware-as-a-service models and AI-assisted phishing tools, accelerating both the frequency and sophistication of attacks. According to industry reporting, healthcare data breaches in 2025 affected tens of millions of individuals, reinforcing that protected health information (PHI) remains a high-value target. The operational consequences of these attacks often extend far beyond data exposure. They can disrupt scheduling, billing, patient communication, and even direct clinical care. For independent practices, this means cybersecurity is not theoretical. It directly impacts continuity of care and revenue stability. We’ve seen firsthand how a single incident can cascade through a practice’s operations, affecting everything from patient appointments to insurance reimbursements. HIPAA Compliance Is Foundational, But Not Enough HIPAA and HITECH establish required safeguards for electronic protected health information (ePHI), including encryption, access controls, audit logs, and breach notification procedures. These standards remain essential in 2026, and every practice must maintain rigorous compliance. However, regulatory compliance alone does not guarantee resilience. Many organizations that experienced breaches in 2025 were technically compliant at the time of the incident. The distinction between compliance and security maturity has become increasingly clear, and it’s a distinction that matters enormously. Compliance answers the question: “Are we meeting regulatory minimums?” Security maturity asks: “Can we prevent, detect, and recover from real-world threats?” Practices must evaluate both. This is why practices should also look beyond HIPAA compliance and ask whether their EHR vendor maintains ONC (Office of the National Coordinator) certification. ONC certification represents a rigorous, independent validation that an EHR system meets federal security and interoperability standards, going beyond baseline regulatory requirements. Not all EHR vendors maintain this certification, making it a meaningful differentiator when evaluating platform trustworthiness and long-term viability. Cloud Architecture and Third-Party Risk Exposure Modern EHR platforms are frequently cloud-hosted, offering scalability, remote accessibility, and improved data redundancy. Yet security vulnerabilities often stem from misconfigurations, outdated software components, or poorly secured APIs. Additionally, interoperability introduces new exposure points. EHR systems routinely connect with clearinghouses, payment processors, laboratories and imaging centers, patient engagement tools, and revenue cycle management systems. Each integration creates a potential access vector if not properly secured and monitored. Healthcare cybersecurity analyses in 2025 identified third-party vendor relationships and configuration errors as persistent sources of breach risk. This reinforces the need for continuous vendor oversight, secure API frameworks (including FHIR-based integrations), and ongoing infrastructure patching. When evaluating EHR vendors, practices should ask not only about compliance certifications but whether the platform maintains active ONC certification. This ongoing commitment signals that a vendor invests continuously in meeting evolving federal security and interoperability standards, a marker of both technical rigor and organizational accountability. Security in 2026 requires architectural discipline, not just software functionality. At ClinicMind, we emphasize that practices should know exactly how their data flows through their technology ecosystem and who has access at each stage. Human Behavior Remains a Leading Risk Factor Despite technological advances, phishing attacks, stolen credentials, and improper access controls continue to drive healthcare security incidents. Weak passwords, shared logins, and insufficient staff training remain common contributors to breaches. Multi-factor authentication (MFA), role-based access controls, and structured internal policies significantly reduce exposure, yet adoption remains inconsistent across smaller practices. Cybersecurity experts emphasize that technology alone cannot compensate for weak operational governance. Leadership engagement, consistent staff education, and regular security reviews are essential components of a mature EHR security posture. In short, security is not a feature that can be “installed.” It is a system that must be maintained, and that maintenance requires commitment from leadership and accountability across the entire organization. Data Security as a Strategic Business Decision In 2026, EHR data security affects far more than compliance audits. It directly influences patient trust, payer relationships, reimbursement continuity, malpractice and cyber liability exposure, and practice valuation and growth readiness. Healthcare organizations that invest in resilient security infrastructure position themselves to withstand disruption and scale confidently. As practices evaluate their security posture, they should ask themselves: Is the EHR platform built on a continuously updated architecture? Does the vendor maintain ONC certification, demonstrating commitment to federal security and interoperability standards? Are penetration testing and security audits conducted regularly? Is there transparent incident response planning? How are third-party integrations monitored? Are backups and disaster recovery protocols tested? The practices asking these questions proactively, rather than reactively, will be best positioned for sustainable growth. This is where security becomes strategy: the practices that move first to strengthen their defenses gain competitive advantage in attracting patients, partners, and investors. Final Perspective: Security as Infrastructure for Stability Healthcare digital transformation will continue to accelerate. AI documentation tools, interoperability mandates, and cloud adoption will further increase system complexity. But complexity without discipline creates risk. The practices that thrive in 2026 and beyond will treat EHR data security not as a compliance checkbox, but as foundational infrastructure for clinical reliability and financial continuity. They’ll also be intentional about partnering with vendors, like those maintaining ONC certification, who demonstrate genuine, ongoing commitment to security excellence. At ClinicMind, we believe security is ultimately about enabling practices to focus on what they do best: delivering
PatientHub vs SKED: Which Platform Helps Chiropractic Clinics Grow Faster?

PatientHub vs SKED: Which Platform Helps Chiropractic Clinics Grow Faster? Modern chiropractic practices need more than appointment reminders. They need systems that fill schedules, reactivate patients, answer calls, and reduce administrative load — without adding staff.SKED has helped many chiropractors automate text reminders and online booking. PatientHub, part of the ClinicMind platform, goes further by combining AI communications, automated reactivation, online scheduling, two-way SMS, and virtual phone answering inside a single EHR and billing ecosystem. Both tools serve the same mission: help chiropractic practices stay connected with patients and reduce no-shows. The difference is scope and depth. Below is a clear breakdown to help you choose the right solution for your practice. Quick Verdict Choose SKED if you are a single-location, cash-based, or early-stage chiropractic practice looking primarily for appointment reminders and simple online scheduling. Choose PatientHub if you want automated patient engagement, AI receptionist capabilities, and measurable reactivation results — fully integrated with your EHR and billing workflows. PatientHub is built for clinics that want to automate more, avoid missed calls, re-engage dormant patients, and support multi-provider growth with less administrative overhead. We Listen. Then We Build. Every feature inside PatientHub exists because practices share their challenges, their hopes, and their daily frustrations. We didn’t guess what you needed – we designed PatientHub by listening carefully. “We needed scheduling that just works – across every provider.” You told us how hard it was to keep multiple calendars in sync and avoid double bookings.So we built Service Calendars – a fully integrated scheduling system that connects directly with your ClinicMind EHR. No third-party workarounds, no manual updates, just smooth, reliable scheduling for every provider and location. “Every appointment, every provider, perfectly aligned.” “We kept missing calls after hours – and it cost us patients.” We understand how painful that is. That’s why PatientHub includes Voice AI and AI Chat, virtual assistants that never sleep. They answer calls, book appointments, respond to messages, and handle FAQs 24/7, giving your staff peace of mind and patients instant service. Feature Comparison Features PatientHub SKED Why It Matters Two-way SMS ✅ ✅ Reduce no-shows & quick patient replies Online booking ✅ ✅ Simple patient scheduling AI voice answering ✅ 24/7 ❌ Don’t miss calls or new patients AI chat assistant ✅ ❌ Instant help for patients online Automated reactivation ✅ ❌ Recover dormant patients automatically EHR-integrated ✅ Native ❌ Standalone Single source of truth Consent + compliance audit ✅ Limited Documentation + billing alignment Multi-location / providers ✅ Limited Essential for scaling Analytics & revenue proof ✅ Basic Measure ROI, not just reminders Common Feedback From SKED Users Across multiple third-party review platforms, users consistently highlight a few recurring areas where SKED could improve. Areas for Improvement Upload Reliability: Some users report occasional upload issues that require manual posting or additional steps. Analytics Depth: While analytics meet basic needs, some users prefer relying on Facebook’s native tools and note limited depth within SKED. These themes don’t diminish SKED’s value as a scheduling and reminder tool, but they do point to limitations for clinics looking for deeper automation, clearer performance tracking, and measurable growth outcomes — areas where PatientHub is purpose-built to go further. “We wanted a way to bring patients back — automatically.” This was one of the biggest requests we heard.So, we created Reactivation AI — an automated engine that identifies inactive patients, sends personalized messages, and tracks the revenue recovered from every campaign. The results have been remarkable: 83% average increase in reactivations $12K–$24K in recovered revenue within the first campaign ROI visible in as little as 3 weeks — with no new staff or marketing budgetPH _ Sked_ Presentation Pitch “We wanted to actually see the impact.” PatientHub’s Reactivation Dashboard brings that clarity to life.You can track reactivated patients, measure booked vs. potential revenue, and identify your top-performing campaigns, all in real time. “We needed to communicate without juggling five tools.” We get it. That’s why PatientHub connects everything.Your texts, emails, voicemails, and even review replies all live in one place – so your team never misses a message or loses context. And because it’s part of the ClinicMind ecosystem, everything stays HIPAA-compliant and fully synchronized with your patient records. “We wanted tools that help us grow, not just manage.” You asked for tools that don’t just automate tasks, but create opportunities.So, we added AI-powered marketing and growth features that work seamlessly with your daily operations: AI Review Response Generator – replies automatically and strengthens your online reputation AI Blog and Social Media Tools – generate SEO-ready content in seconds Reputation Booster – prompts happy patients for 5-star reviews Built for Connection, Not Just Convenience At PatientHub, we believe technology should feel human.That’s why every feature was designed to lighten your workload, reconnect patients with care, and give your team back valuable time. And because it’s backed by ClinicMind, you can trust that it’s built for long-term stability and continuous innovation – not short-term fixes. See Results in Just 4 Weeks Most practices see reactivated patients, and new revenue within the first month of using PatientHub. Week Focus Result Week 1 Connect your systems Data synced Week 2 Launch automations Campaigns live Week 3 Patients respond Bookings return Week 4 Measure ROI Dashboard reporting growth Because You Deserve More Than a Scheduler You deserve tools that listen, evolve, and grow with your practice. PatientHub isn’t about replacing what came before — it’s about continuing the story with smarter, simpler, and more human technology. Reactivate Up to 83% of Your Inactive Patients — Automatically Your next wave of growth is already in your patient list.Let’s help you reach them. Book your personalized Reactivation Review to see your hidden revenue potential.Get started today with PatientHub — the smarter way to schedule, engage, and grow. Why Clinics Switch to PatientHub Chiropractic teams report switching when they need to: Stop missing phone calls & new patient opportunities Scale past simple reminders Reduce staff effort on follow-ups and reactivations Connect scheduling to EHR
PatientHub Recognized by G2 for Patient Engagement
PatientHub Recognized by G2 for Patient Engagement When you run a clinic, you don’t measure success by clicks, badges, or even revenue alone. You measure it by the people who keep walking through your door. The mom who finally feels heard. The patient who shows up for every appointment because you made it easy. The person who, after months away, decides to come back because you reached out at just the right time. That’s what patient engagement really is: keeping people connected, engaged, and loyal—because healing happens through relationships. Recently, ClinicMind was recognized by G2 for Patient Engagement. For us, it wasn’t about the award itself—it was about what it meant. Providers are telling the world: this works. Patients are staying connected. Practices are growing, not just through billing, but through trust. At the center of that recognition is PatientHub. The Patient Engagement Challenges Clinics Face The phone rings while your staff is already juggling three patients. A no-show leaves an empty slot and lost revenue. A first-time patient falls through the cracks because no one had time to follow up. After hours, every missed call feels like another missed opportunity. These aren’t small inconveniences—they’re the moments that decide whether a patient stays with you or slips away. How PatientHub Improves Patient Engagement PatientHub was built for this world—the one you live in every day. Here’s how it helps you not just survive, but thrive: 24/7 Patient Communication with Voice AI & Chat: With Voice AI and our 24/7 Chat Bot, every patient gets an answer—even if it’s midnight. Bookings happen instantly. FAQs get handled automatically. No more missed opportunities, no more apologies. Reduce Patient No-Shows with Automated Reminders: Automated reminders by text, email, or voicemail cut no-shows by up to 38%. That means steadier schedules, steadier revenue, and fewer gaps in patient care. Centralized Patient Communication Hub: Instead of chasing emails, voicemails, and texts across different systems, PatientHub gives you a central engagement hub. Every message, every history, every patient—all right where you need it. Patient Reactivation & Nurture Campaigns: Our Reactivation and Nurture Campaigns quietly work in the background, reaching out to patients who haven’t been in for a while and keeping active patients engaged between visits. You focus on care—we handle the follow-up. AI-Powered Patient Reviews & Reputation Management: With AI-powered review responses and automated review boosters, PatientHub makes sure every patient feels heard, while also building the reputation that attracts the next new patient. Why Patient Engagement Tools Matter Today Patients today expect more than appointments—they expect connection. They want to know you’re listening, that you’re available, and that their care doesn’t end when they leave the office. For chiropractors and clinicians, this isn’t about “keeping up with technology.” It’s about staying human in a world that’s moving faster every day. PatientHub doesn’t replace relationships—it protects them. The Real Story Behind the Recognition The G2 recognition wasn’t about us. It was about you—the providers who use PatientHub to turn missed calls into new bookings, empty chairs into filled appointments, and one-time visits into lifelong relationships. Because when patients feel connected, they stay. They heal. They trust. And that’s what PatientHub is really about. Want to see how PatientHub can strengthen your patient relationships? Book a demo and experience what true engagement feels like. Book a free consultation
Credentialing Readiness Assessment Checklist for Healthcare Practices
Use this checklist to see how prepared your practice is for a successful credentialing process. Readiness matters because delays can lead to lost revenue, denials and compliance issues. The more items you check, the smoother your credentialing journey will be. 📁 1. Organizational Information for Credentialing ☐ Legal business name matches IRS records ☐ Tax ID Number (TIN) and NPI are active and valid ☐ Business entity is properly registered (LLC, PC, etc.) ☐ Up-to-date malpractice insurance with correct policy details 👤 2. Provider Documentation Needed for Credentialing ☐ Valid professional license(s) in all practicing states ☐ Board certifications and continuing education records ☐ DEA certificate (if prescribing medications) ☐ State-controlled substance registration (if applicable) ☐ Up-to-date CV (chronological, no unexplained gaps) 📋 3. Practice Operations ☐ Office address and phone number are current ☐ W-9 form is completed and signed ☐ Business hours and services offered clearly documented ☐ Staff roles and titles are defined 💻 4. CAQH, NPPES & Online Credentialing Profiles ☐ CAQH profile is completed and attested ☐ All documents uploaded to CAQH are current ☐ NPPES profile is accurate (NPI registry) ☐ PECOS enrollment is active (for Medicare providers) 💰 5. Insurance Payer-Specific Credentialing Readiness ☐ Target list of insurance payers is created ☐ Knowledge of each payer’s requirements and timelines ☐ Ready to submit applications individually or via delegated credentialing 📦 6. Internal Credentialing Process ☐ Dedicated staff or team for credentialing ☐ Timeline expectations set (90–150 days on average) ☐ Process in place to follow up with payers regularly ☐ Method to track application statuses 📉 7. Risk Factors That Delay Credentialing ☐ No past license suspensions or malpractice issues ☐ Gaps in work history are clearly explained ☐ No disciplinary actions by state boards 🧭 Scoring Your Credentialing Readiness ✅ 24–28 checks: Credentialing-Ready – You’re in great shape to start or streamline your credentialing. ⚠️ 15–23 checks: Partial Readiness – You’re close, but gaps may slow you down or lead to denials. ❌ 0–14 checks: At-Risk – Credentialing delays, rejections, or payer issues are likely without support. 👉 Not Fully Ready? We’ve Got You. CredEdge handles credentialing from start to finish. Document collection, application submission, payer follow-ups, and compliance monitoring. 🎯 Get Expert Help with Credentialing
Why ClinicMind Wins G2 Fall 2025 Awards for EHR, Billing & Patient Engagement
When you’re running an independent practice, software badges probably aren’t top of mind. What matters is whether your team can keep up with documentation, whether your reimbursements arrive on time, and whether your patients stay committed. That’s the real story behind ClinicMind’s G2 Fall 2025 recognition. Yes, we earned nine new awards across 20 categories, extending our leadership streak to 13 straight quarters and 35 total badges this year. But the badges aren’t the point. They’re simply proof of what happens when providers replace disconnected “Frankenstacks” with one unified growth platform. From Disconnected Tools to a Unified EHR & Billing Platform Too many practices still rely on pieced-together systems: one for billing, another for notes, a third for patient reminders, plus a maze of spreadsheets. Each gap creates additional administrative work, increased payer delays, and more opportunities for revenue to be lost. ClinicMind was built to end that cycle. By bringing credentialing, billing, documentation, and patient engagement into a single compounding suite, we help providers: Recover revenue with faster, cleaner claims. Shrink admin time so staff can focus on patients. Boost retention with built-in engagement tools that keep patients connected. ClinicMind G2 Fall 2025 Awards: Real Recognition That Matters G2 users confirmed what our clients tell us every day: Momentum in billing and EHR shows practices are actively switching to unlock lost revenue. Leadership in chiropractic means providers can finally document faster and stay compliant without drowning in paperwork. High performance in small-business billing & EHR proves even lean teams can run like big ones. Recognition in patient engagement signals that growth isn’t just billing, it’s stronger patient relationships. And perhaps the most meaningful validation? The “Users Love Us” badge. That one can’t be bought; it comes directly from providers who’ve experienced the shift firsthand. What G2 Recognition Means for Your Practice Awards are nice, but no one buys software for a badge. The real win is when: Your staff feels less burned out. Your reimbursements arrive predictably. Your patients keep coming back. That’s what ClinicMind delivers and why recognition keeps compounding. See Why Practices Switch to ClinicMind Book your free consultation today and discover how one platform can replace your Frankenstack and protect your revenue. Read the full details in our official G2 Fall 2025 press release
How ClinicMind’s RCM Software + Service Reduced A/R Over 120 to 4%
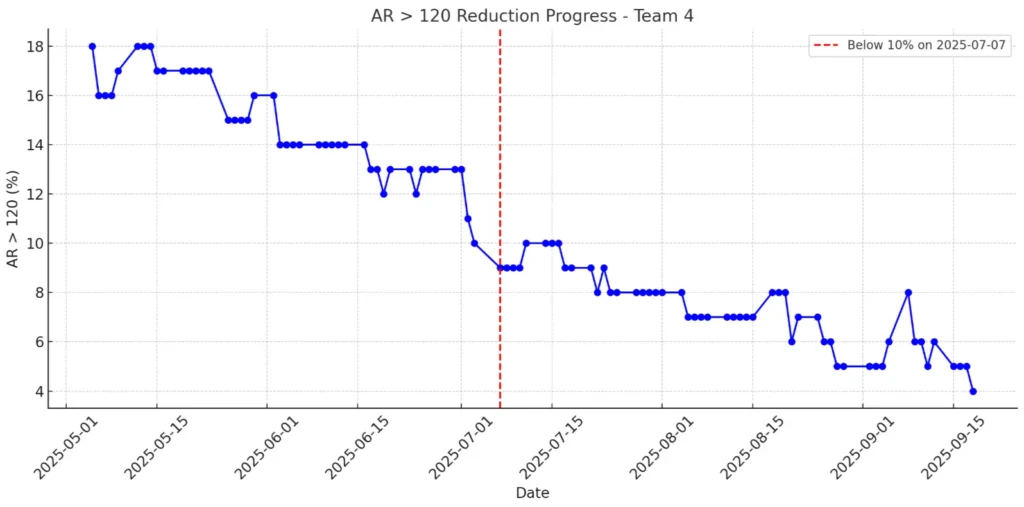
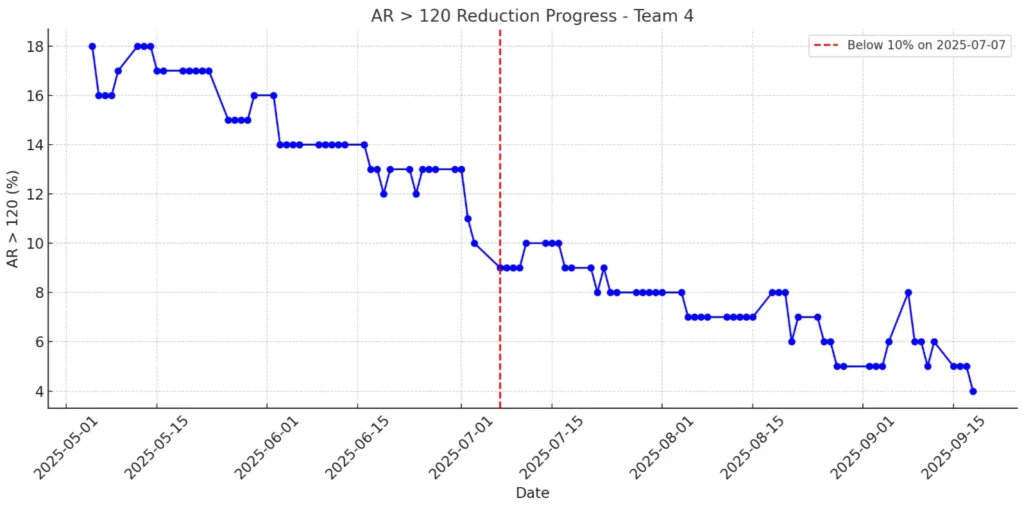
How ClinicMind’s RCM Software + Service Reduced A/R Over 120 to 4% In healthcare revenue cycle management (RCM), results are what count. Achieving numbers like these is rare. ClinicMind’s RCM Team recently reached an A/R over 120 days of just 4%, which is only a third of the industry average of 13.4% according to MGMA. This milestone didn’t happen by chance. It came from ClinicMind’s approach of blending strong RCM software with skilled human support. This system helps practices lower their aged A/R and speed up cash flow. What is A/R > 120, and Why Does It Matter? Accounts Receivable (A/R) aged beyond 120 days represents money practices may never collect. The higher the percentage, the greater the financial strain. With the industry benchmark sitting at 13.4%, many practices face delayed or lost revenue. ClinicMind’s Team kept their rate at just 4%, showing that practices can reach and maintain top results when they have the right tools and expertise. From 13% to 4%: ClinicMind’s 60-Day A/R Reduction Journey Late June 2025 Team was at 13%, aligned with MGMA benchmarks. In July 2025, our numbers improved steadily, moving from 12% to 9%, then 7%, and finally 6%. By August 2025, we held steady between 5% and 7%, finishing the month at 4%. Within 60 days, we cut our aged A/R in half and kept it at that level. ClinicMind RCM Software: Automating Revenue Cycle Management Our software helps you work more accurately, saves time with automation, and keeps everything clear. Daily RCM Dashboards: The 4% metric itself came from real time ClinicMind dashboards, providing transparency for clients and teams alike. Automated Denial Alerts: Same-day appeal workflows were triggered instantly by software, preventing delays. Bulk Patient Statements: Automated statement generation and small balance sweeps ensured no revenue was overlooked. Account Prioritization: Smart filters highlighted high-balance accounts, allowing teams to focus on the most critical accounts first. Expert RCM Services that Deliver Results Same-Day Appeals: Analysts acted immediately on flagged denials. Collector Focus: Experienced team members handled the top 20 high-balance accounts directly. Backlog Blitz: Analysts were temporarily reassigned to address the A/R over 120-day backlog. They worked at scale based on insights from the dashboards. The Result: Software created visibility and automation; the service team applied judgment, persistence, and expertise. This balance of technology and expert support is what makes ClinicMind a leader in healthcare revenue cycle management and RCM billing services. Why ClinicMind’s A/R Performance Matters for Practices Benchmark Beating: 4% vs. 13.4% shows ClinicMind delivers world-class outcomes. Consistency: This was not just a brief improvement. The ongoing performance trend shows that these results are sustainable. Scalability: The same playbook of software + service can be replicated across other teams and client BPOs. By combining RCM software with expert human support, ClinicMind helps practices achieve world-class revenue cycle optimization Software + Service = Sustainable RCM Success Technology by itself can’t fix revenue cycle challenges, and service alone won’t scale without the right data and automation. ClinicMind’s story shows that when smart software and expert service work together, the financial results are hard to beat. See how your practice can achieve industry-leading A/R results with the right technology and expert support – Book a consultation to learn more
How ClinicMind’s RCM Software + Service Reduced A/R Over 120 to 4%