Healthcare Practice Management Statistics – 2026
Independent practices are under growing pressure as administrative demands rise, margins tighten, and disconnected systems limit performance. This report brings together market benchmarks, adoption trends, and operational data to show what is driving growth, where revenue is being lost, and which inefficiencies are holding practices back. For many organizations, the challenge is not effort, but fragmentation across scheduling, documentation, billing, credentialing, and patient communication systems. When these functions operate separately, the impact is clear: slower revenue cycles, greater staff strain, and less room for sustainable growth. This report highlights where those gaps appear and why more practices are turning to integrated platforms to improve efficiency, visibility, and financial outcomes. Healthcare Practice Management Market Size, 2026 The practice management market is expanding because healthcare organizations are no longer looking for one more tool. They are looking for systems that reduce operational drag, improve financial performance, and support long-term growth. Market Segment 2025 Market Value 2026 Projected Value 2033 Projection CAGR Practice Management Software (Global) $17.02B $18.70B $42.37B 9.86% Practice Management Software (U.S.) $5.89B $6.38B $11.24B 8.3% Physician Practice Management Services $118.9B $129.5B $291.7B 9.2% Digital Health Technology (Overall) $278B $312B — 12.2% Key Research Findings: Growth is strongest in solutions that combine software and services, signaling a clear market shift. Practices are looking for more than disconnected tools. They want support for operational functions that directly impact revenue, including: Billing Credentialing, and patient engagement. The U.S. continues to account for a disproportionate share of spending due to greater: Billing complexity Payer friction, and compliance pressure. Small and midsize practices are helping drive adoption as they look for ways to grow without adding administrative burden. Technology Adoption Rates in Healthcare Practices, 2026 Technology adoption is increasing across the industry, but the gap between large organizations and independent practices remains significant. The practices moving fastest are the ones investing in systems that improve efficiency across the full operation, not just one department at a time. Technology Overall Adoption Large Systems (50+ providers) Small Practices (1-10 providers) Avg. Implementation Time Electronic Health Records (EHR) 94% 99% 87% 8-12 months Telemedicine Platforms 82% 91% 73% 3-6 months Patient Portals 78% 89% 62% 4-8 months Remote Patient Monitoring 67% 84% 45% 6-10 months AI-Powered Documentation 54% 73% 28% 12-18 months Integrated RCM (Revenue Cycle Management) 61% 82% 48% 6-14 months Automated Patient Engagement 59% 77% 41% 4-7 months Credentialing Management Software 43% 68% 29% 3-6 months Key Research Findings: Larger health systems continue to outpace smaller practices in adoption, gaining advantages in: Speed Consistency, and patient experience. AI-powered documentation saw the fastest growth, driven by the need to: Reduce provider burnout Reclaim time lost to charting. Practices using integrated systems report: Stronger staff satisfaction Lower operational costs. These outcomes outperform those reported by practices relying on fragmented technology stacks. Practice Management Technology ROI and Performance Metrics, 2026 Technology should do more than add functionality. It should help practices recover time, reduce friction, and create a measurable lift in revenue performance. The strongest returns come from systems that connect core workflows instead of isolating them. Technology Avg. ROI Timeline Cost Reduction Efficiency Gain Revenue Impact Clinical Outcome Improvement Integrated Practice Platform 6-10 months 25-32% 38% +18-24% +12% AI-Powered Documentation 24 months 15% 40% +8-12% +25% Automated Patient Engagement 8 months 18% 35% +14-19% +12% Revenue Cycle Management (RCM) 14 months 22% 30% +16-28% +8% Credentialing Automation 4-7 months 12-18% 45% +12-22% — Electronic Health Records (EHR Only) 18 months 12% 25% +6-9% +8% Key Research Findings: Integrated platforms deliver faster ROI by removing friction across multiple workflows at once. When documentation, billing, and patient engagement work together, practices see gains sooner and across more areas of the business. The returns from integrated systems build over time. Practices that adopt integrated systems can: Pmprove collections Reduce delays Strengthen retention Free up provider capacity. Together, these gains create a compounding effect on growth. Healthcare Practice Operational Benchmarks, 2026 Operational performance tells a clear story. Practices with stronger revenue outcomes are not simply working harder, they are operating with fewer handoff points, cleaner workflows, and better systems. Metric Top Quartile (Top 25%) Median Bottom Quartile (Bottom 25%) Patient No-Show Rate 4-7% 12-15% 22-28% Days in Accounts Receivable (A/R) 24-32 days 45-52 days 68-85 days Clean Claim Rate (First-Pass Acceptance) 92-96% 78-84% 62-71% Net Collection Rate 96-98% 82-88% 68-76% Provider Utilization Rate 82-88% 68-74% 52-62% Patient Retention Rate (12-Month) 78-84% 58-65% 38-47% Revenue Per Provider (Annual) $620K-$840K $420K-$540K $280K-$380K Technology Systems in Use 1-2 platforms 3-5 platforms 6-9 platforms Key Research Findings: Fragmentation remains a direct driver of revenue leakage. Practices using more disconnected systems report: Higher no-show rates Slower collections Weaker financial performance. The highest-performing practices generate significantly more revenue per provider. Their stronger performance is driven in large part by their ability to: Retain patients more effectively Submit cleaner claims, Keep operations moving without unnecessary friction. Practice Management Technology Implementation Challenges, 2026 Adopting better technology can transform performance, but implementation often fails when practices underestimate the operational side of change. Success depends on support, clarity, and a rollout process the team can actually absorb. Implementation Challenge Frequency Impact on Success Rate Avg. Time to Resolve Staff Resistance to Change 73% -34% 6-9 months Budget Constraints 68% -28% 3-6 months Technical Integration Issues 61% -41% 4-12 months Data Migration Complexity 58% -38% 2-6 months Insufficient Vendor Support 54% -45% Ongoing Lack of Internal IT Resources 49% -22% 3-8 months Unclear ROI Expectations 42% -19% 1-3 months What Improves Adoption Success: Practices are more likely to succeed when they: Invest in training Work with vendors that provide hands-on support Roll out changes in phases rather than all at once The technology matters, but the implementation model matters just as much. Platform design and vendor alignment are critical to successful adoption. When the system is unified and the support team understands the full workflow, adoption becomes: Simpler Faster Less disruptive. Healthcare Practice Growth Trends and Market Dynamics, 2026 The direction of the market is clear. Practices are moving away from disconnected
Medical Billing Statistics, 2026 Report
Medical billing errors affect millions of Americans annually, with consequences extending beyond immediate financial strain to long-term credit impacts and delayed medical care. The data presented below reflects patterns observed across insurance types, age groups, and healthcare settings, with particular attention to error rates, collection practices, and patient advocacy outcomes. Key Findings: 80% of medical bills contain at least one error, making billing mistakes the norm rather than the exception across the U.S. healthcare system $88 billion in medical debt appears on American credit reports annually, with 58% of all collection accounts stemming from healthcare bills Insurance claim denials are processed in an average of 1.2 seconds through automated systems like Cigna’s PXDX, often without meaningful review of patient records 74% of patients who dispute billing errors successfully get them corrected, yet 86% of those who don’t contact billing offices assume it wouldn’t make a difference 98% of older adults with unpaid medical bills have health insurance, demonstrating that coverage alone doesn’t protect against billing problems Most billing disputes require less than one hour of patient time, contradicting the common perception that challenging medical bills is prohibitively time-consuming Medical Billing Error Rates and Financial Impact The prevalence of medical billing errors remains alarmingly high across the U.S. healthcare system. Recent data reveals that the majority of medical bills contain at least one error, contributing to billions in disputed charges annually. Metric Value Medical bills containing errors 80% Insured adults receiving unexpected medical bills 45% Annual medical debt on credit reports $88 billion U.S. households with medical debt 20% Bills in collections that are medical bills 58% Insurance Claim Denials and Coverage Disputes Insurance companies employ increasingly automated systems to review and deny claims, often without thorough examination of patient records. The speed and volume of denials have accelerated significantly. Metric Value Coverage denials for physician-recommended services 17% Patients experiencing care delays from denials 60% Patients with health deterioration due to denials 47% Claims denied by private insurers 1 in 7 Cigna claims denied via PXDX system (2-month period) 300,000+ Average time per PXDX denial decision 1.2 seconds Formal appeals filed for ACA marketplace denials 0.1% Medical Billing Among Older Americans Older adults with Medicare coverage face unique billing challenges despite near-universal insurance coverage. The complexity of coordinating multiple payers and frequent medical care creates opportunities for billing errors. Metric Value Adults 65+ with unpaid medical bills (2020) 3.9 million Older adults with unpaid bills who have insurance 98% Older adults with unpaid bills covered by 2+ insurers 70% Total unpaid medical bills, adults 65+ $53.8 billion Year-over-year increase (2019-2020) 20% Average unpaid bill amount, adults 65+ $13,800 Medicare/Medicaid dual beneficiaries with unpaid bills 10% Patient Success Rates When Disputing Medical Bills Challenging medical bills can yield substantial financial relief, yet many patients never attempt to dispute charges. Recent research quantifies the outcomes for those who do take action. Metric Value People receiving problematic medical bills 1 in 5 Recipients who contacted billing office 61.5% Patients who had billing errors corrected 74% Patients receiving financial relief for unaffordable bills 76% Patients who successfully negotiated price reductions 62% Overall success rate (any positive outcome) 1 in 4 Medicare beneficiaries with favorable outcomes 61% Medicaid beneficiaries with favorable outcomes 46% Non-contactors who believed it wouldn’t help 86.1% Patient Barriers to Challenging Medical Bills Despite high success rates when disputing bills, significant barriers prevent many patients from seeking corrections or financial assistance. Awareness gaps and demographic disparities affect who attempts to challenge charges. Demographic/Factor Likelihood to Contact Billing Office Adults without college degree Lower Adults with lower financial literacy Lower Uninsured adults Lower Adults aged 19-34 unaware of dispute rights 60% All adults uncertain if they could challenge bills 54% Adults uncertain how to appeal or who to contact 40% Higher-income adults citing lack of time 23% Time required to dispute (most cases) <1 hour Credit Impact and Long-Term Consequences Medical billing errors that progress to collections can devastate patient credit scores and financial futures, with disproportionate impacts on communities of color and low-income households. Metric Value Older adults with medical collections tradelines 5.1 million Total medical collection debt on credit reports (65+) $7.97 billion Patients who experience worry/anxiety from denials 80% National health expenditures (2023) $4.8 trillion U.S. health spending going to chronic conditions 90% Credit score improvement from updated models 25 points About This Report This comprehensive report was developed for ClinicMind. Sources Consumer Financial Protection Bureau — Medical Billing and Collections Among Older Americans Author: CFPB Office for Older Americans Publication Date: May 30, 2023 URL: https://www.consumerfinance.gov/data-research/research-reports/issue-spotlight-medical-billing-and-collections-among-older-americans/ The Commonwealth Fund — Unforeseen Health Care Bills and Coverage Denials by Insurers Authors: Gupta A, Collins SR, Roy S, Masitha R Publication Date: August 1, 2024 URL: https://www.commonwealthfund.org/publications/issue-briefs/2024/aug/unforeseen-health-care-bills-coverage-denials-by-insurers USC Schaeffer Center for Health Policy & Economics — Challenging Medical Bills Study Lead Author: Erin L. Duffy Publication Date: August 30, 2024 Published in: JAMA Health Forum URL: https://schaeffer.usc.edu/research/challenging-medical-bills-cost-study/ Centers for Medicare & Medicaid Services (CMS) — Medical Bill Rights URL: https://www.cms.gov/medical-bill-rights/help/guides/bill-errors ProPublica — Cigna PXDX Investigation Authors: Rucker P, Miller M, Armstrong D Publication Date: March 25, 2024 Kaiser Family Foundation — Claims Denials and Appeals in ACA Marketplace Plans Authors: Politz K, Lo J, Wallace R, Mengistu S Publication Date: February 9, 2024
How ClinicMind’s RCM Software + Service Reduced A/R Over 120 to 4%
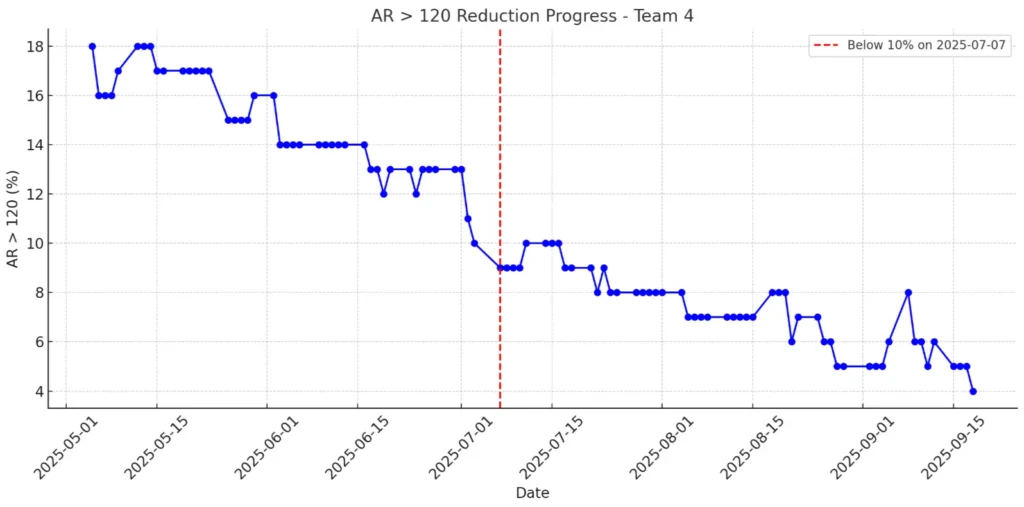
How ClinicMind’s RCM Software + Service Reduced A/R Over 120 to 4% In healthcare revenue cycle management (RCM), results are what count. Achieving numbers like these is rare. ClinicMind’s RCM Team recently reached an A/R over 120 days of just 4%, which is only a third of the industry average of 13.4% according to MGMA. This milestone didn’t happen by chance. It came from ClinicMind’s approach of blending strong RCM software with skilled human support. This system helps practices lower their aged A/R and speed up cash flow. What is A/R > 120, and Why Does It Matter? Accounts Receivable (A/R) aged beyond 120 days represents money practices may never collect. The higher the percentage, the greater the financial strain. With the industry benchmark sitting at 13.4%, many practices face delayed or lost revenue. ClinicMind’s Team kept their rate at just 4%, showing that practices can reach and maintain top results when they have the right tools and expertise. From 13% to 4%: ClinicMind’s 60-Day A/R Reduction Journey Late June 2025 Team was at 13%, aligned with MGMA benchmarks. In July 2025, our numbers improved steadily, moving from 12% to 9%, then 7%, and finally 6%. By August 2025, we held steady between 5% and 7%, finishing the month at 4%. Within 60 days, we cut our aged A/R in half and kept it at that level. ClinicMind RCM Software: Automating Revenue Cycle Management Our software helps you work more accurately, saves time with automation, and keeps everything clear. Daily RCM Dashboards: The 4% metric itself came from real time ClinicMind dashboards, providing transparency for clients and teams alike. Automated Denial Alerts: Same-day appeal workflows were triggered instantly by software, preventing delays. Bulk Patient Statements: Automated statement generation and small balance sweeps ensured no revenue was overlooked. Account Prioritization: Smart filters highlighted high-balance accounts, allowing teams to focus on the most critical accounts first. Expert RCM Services that Deliver Results Same-Day Appeals: Analysts acted immediately on flagged denials. Collector Focus: Experienced team members handled the top 20 high-balance accounts directly. Backlog Blitz: Analysts were temporarily reassigned to address the A/R over 120-day backlog. They worked at scale based on insights from the dashboards. The Result: Software created visibility and automation; the service team applied judgment, persistence, and expertise. This balance of technology and expert support is what makes ClinicMind a leader in healthcare revenue cycle management and RCM billing services. Why ClinicMind’s A/R Performance Matters for Practices Benchmark Beating: 4% vs. 13.4% shows ClinicMind delivers world-class outcomes. Consistency: This was not just a brief improvement. The ongoing performance trend shows that these results are sustainable. Scalability: The same playbook of software + service can be replicated across other teams and client BPOs. By combining RCM software with expert human support, ClinicMind helps practices achieve world-class revenue cycle optimization Software + Service = Sustainable RCM Success Technology by itself can’t fix revenue cycle challenges, and service alone won’t scale without the right data and automation. ClinicMind’s story shows that when smart software and expert service work together, the financial results are hard to beat. See how your practice can achieve industry-leading A/R results with the right technology and expert support – Book a consultation to learn more
The Compound Effect of Simultaneous Growth in Patient Attraction, Average Patient Value, and Billing Performance Quality
In the world of healthcare practices, sustainable growth requires more than just delivering excellent care—it demands a strategic approach to increasing revenue and operational efficiency. To achieve consistent and scalable growth, practices can focus on improving three critical areas simultaneously: patient attraction, average patient value (APV), and billing performance quality. The synergistic effect of advancing these pillars creates a compounding impact that accelerates the practice’s success. 1. Patient Attraction: The Gateway to Growth Patient attraction is the foundation of a thriving healthcare practice. Without a steady influx of new patients, growth stagnates, and opportunities for increasing revenue diminish. Strategies for Improving Patient Attraction: Digital Presence: Build a robust online presence through a well-designed website, active social media engagement, and local search optimization. Reputation Management: Encourage satisfied patients to leave reviews and testimonials. Positive reviews build trust and attract new patients. Community Outreach: Partner with local businesses, schools, or organizations to raise awareness of your services. Specialized Services: Offer niche or advanced procedures that differentiate your practice from competitors. The more effectively you attract patients, the larger your pool for implementing improvements in the other two areas—APV and billing performance. 2. Average Patient Value: Maximizing the Patient Relationship Once patients are in the door, the focus shifts to increasing their lifetime value to the practice. APV measures the revenue each patient generates over time. By optimizing APV, practices ensure they’re making the most of every patient interaction. Strategies for Enhancing APV: Upselling and Cross-Selling: Educate patients about complementary or advanced treatment options that enhance their care experience and outcomes. Membership Programs: Offer subscription-based plans for routine services to encourage patient loyalty and consistent revenue streams. Continuity of Care: Implement systems to schedule follow-up visits, ensuring ongoing patient engagement and treatment adherence. Patient Education: Empower patients with knowledge about their conditions and available treatments, fostering trust and encouraging higher-value care decisions. Increasing APV not only boosts revenue but also strengthens patient relationships, creating ambassadors who promote your practice organically. 3. Billing Performance Quality: Ensuring Financial Efficiency Revenue cycle management (RCM) is often overlooked as a growth driver, but effective billing practices ensure that every dollar earned is collected promptly and accurately. Billing performance quality directly impacts cash flow and profitability. Strategies for Improving Billing Performance: Automation Tools: Invest in software that streamlines billing, reduces errors, and accelerates claim submissions. Training and Development: Regularly train staff on coding updates, insurance guidelines, and patient communication. Transparent Pricing: Offer clear, upfront pricing to minimize patient confusion and improve collections. Data Analysis: Monitor key performance indicators (KPIs) like denial rates, days in accounts receivable (AR), and collection rates to identify and address inefficiencies. A well-oiled billing system allows practices to reinvest resources into patient attraction and care enhancements, fueling further growth. The Compound Effect: How These Pillars Amplify Each Other When practices focus on all three areas simultaneously, the growth potential multiplies. Here’s how the compounding effect works: Enhanced Patient Experience: Improved APV strategies often include better communication, education, and follow-up care, which naturally attract more patients through word-of-mouth referrals. Increased Operational Capacity: Efficient billing improves cash flow, enabling investments in marketing and patient-centric technologies that further boost attraction and APV. Scalable Growth: A higher APV means more revenue per patient, reducing the pressure to attract massive numbers of new patients to achieve financial goals. By aligning efforts in these areas, practices create a self-reinforcing growth loop. New patients bring in revenue, efficient billing optimizes cash flow, and higher APV ensures each patient contributes more to the practice’s success. Final Thoughts: A Blueprint for Sustainable Growth To create compounding growth, practices must take a strategic, data-driven approach. Start by assessing your current performance in patient attraction, APV, and billing. Identify opportunities for improvement, set measurable goals, and invest in tools and training to support your team. When these pillars work together, the results are transformative. Not only will your practice grow, but it will also create a sustainable, patient-centric business model that thrives in any healthcare environment. By committing to continuous improvement, you can unlock the full potential of your practice and achieve lasting success.
Make Payments a Competitive Advantage for Your Practice

In the fast-evolving world of healthcare, efficiency is critical. From patient care to administrative tasks, every second counts. One area where practices often struggle is managing patient payments. Multiple systems, manual entry, and clunky payment processes create unnecessary bottlenecks for practices and headaches for patients. So, how can healthcare providers overcome these challenges? Introducing ClinicMindPay, our newly launched integrated payment processing solution that seamlessly integrates with ClinicMind’s EHR and practice management system. Designed to simplify the payment experience for both patients and practices, ClinicMindPay offers the flexibility, security, and convenience that healthcare practices need to thrive in today’s competitive landscape. Why Should Practices Use ClinicMindPay? If you manage a healthcare practice, you’re likely familiar with the challenges surrounding payment processing. Whether it’s dealing with delayed payments, reconciling invoices manually, or navigating multiple platforms, these inefficiencies add unnecessary complexity to your day-to-day operations. Payment management is often a time-consuming process that can take your focus away from patient care. That’s where ClinicMindPay comes in. Powered by Fortis’ proven technology, ClinicMindPay not only streamlines payments but also fully integrates with ClinicMind’s suite of solutions. Imagine never having to worry about missing payments or spending hours entering data. With ClinicMindPay, your payments sync effortlessly, giving you time back to focus on what matters most—your patients. How ClinicMindPay Solves Payment Challenges Complete Integration: One of the standout features of ClinicMindPay is its seamless integration into your existing ClinicMind EHR and practice management system. Payments are automatically recorded and tracked, reducing administrative workload and minimizing errors. Patient Convenience: In today’s digital world, patients expect convenience. ClinicMindPay allows your patients to pay using their preferred method—whether it’s a credit card, ACH, or even digital wallets—making it easier for them to settle their bills quickly and efficiently. Secure and Reliable: Security is paramount in healthcare, and ClinicMindPay is built with that in mind. Our platform offers top-notch security features to ensure that all transactions are processed safely, providing peace of mind for both you and your patients. Streamlined Reporting: With comprehensive reporting tools, ClinicMindPay makes it easy to track payments, generate reports, and gain insights into your revenue cycle. The result? A more organized, efficient, and financially healthy practice. The Transition for Fortis Clients For our valued Fortis users, the transition to ClinicMindPay is effortless. You won’t need to do anything—your account will be automatically migrated to ClinicMindPay, and you’ll continue to enjoy the same reliable payment services, now with deeper integration into ClinicMind’s suite of solutions. Why Choose ClinicMindPay? ClinicMindPay reflects our dedication to delivering a seamless, all-in-one solution for managing payments. More than just a payment platform, it’s an integrated tool crafted to streamline your operations, enhance patient satisfaction, and boost overall efficiency in your practice. If you’re ready to simplify your payment processes and enhance your practice’s financial health, ClinicMindPay is the solution you’ve been waiting for. For more information on ClinicMindPay and how it can benefit your practice, visit our ClinicMindPay page. You can also check out our full press release to dive deeper into how ClinicMindPay is transforming payment solutions for healthcare providers. Read the press release here.
Transforming Healthcare Billing: How ClinicMind’s Billing Depot Addresses Current Challenges

In today’s fast-paced healthcare landscape, the need for efficient and secure billing solutions has never been more critical. Recent events, such as the cyberattack on UnitedHealth Group, have highlighted vulnerabilities in the healthcare sector, raising questions about data security and the integrity of billing practices. As healthcare providers navigate these challenges, ClinicMind’s Billing Depot emerges as a vital tool in modern practice management. Understanding the Current Landscape The UnitedHealth Group cyberattack serves as a wake-up call for healthcare organizations, reminding them of the importance of robust cybersecurity measures. With sensitive patient data at risk, healthcare providers must prioritize security without sacrificing efficiency. Billing systems are often prime targets for cybercriminals, making it essential for practices to adopt solutions that not only streamline billing processes but also safeguard sensitive information. Why Choose Billing Depot? ClinicMind’s Billing Depot offers a comprehensive billing management solution tailored to the needs of healthcare providers. Here are several key features that set Billing Depot apart, especially in light of current events: Enhanced Security Protocols: ClinicMind’s Billing Depot employs state-of-the-art security measures to protect patient data. This includes encryption, secure access controls, and regular audits to ensure compliance with industry standards. In a time when cyber threats are prevalent, these features provide peace of mind for both providers and patients. Streamlined Workflow: The software simplifies the billing process, reducing administrative burdens. By automating tasks like claim submissions and payment tracking, ClinicMind’s Billing Depot allows healthcare professionals to focus on patient care rather than paperwork. This efficiency is particularly important as practices adapt to increasing patient loads and changing regulations. Real-Time Analytics: With integrated analytics tools, ClinicMind’s Billing Depot empowers practices to make informed financial decisions. Providers can track revenue cycles, identify trends, and optimize their billing strategies. This data-driven approach is crucial for navigating the financial uncertainties posed by ongoing healthcare challenges. Patient-Centric Approach: ClinicMind’s Billing Depot enhances patient engagement through transparent billing processes. Clear communication regarding charges and payments fosters trust, which is essential in a time when patients are more conscious of healthcare costs. Scalability: As healthcare practices grow or adapt to new challenges, ClinicMind’s Billing Depot scales to meet evolving needs. This flexibility is particularly valuable for organizations responding to shifting regulations and market demands. Staying Ahead of Industry Trends The healthcare industry is continually evolving, influenced by technological advancements and regulatory changes. As practices seek to stay competitive, tools like ClinicMind’s Billing Depot can make a significant difference. By integrating advanced billing solutions, providers can not only enhance operational efficiency but also strengthen their resilience against potential cyber threats. In conclusion, ClinicMind’s Billing Depot is not just a software solution; it’s a partner in navigating the complexities of healthcare billing in a rapidly changing environment. As the industry faces challenges like cyberattacks and financial pressures, embracing innovative technology can lead to improved outcomes for both providers and patients. Ready to transform your practice’s billing process? Discover how ClinicMind’s Billing Depot can enhance your efficiency, security, and patient satisfaction. Book a Demo Now! https://clinicmind.com/billing-depot-billing-practice-management-page/
Important Modern Insights and Research into Pre- and Post-Payment Audits

The relationship between pre-bill and post-bill auditing forms a cohesive integration in the revenue cycle. Pre-bill audits prevent errors, boost efficiencies, and safeguard revenue, while post-payment audits provide retrospective insights into navigating payer disputes with evidence-based knowledge. The following developments in technology and innovation have enhanced the effectiveness and efficiency of audits. By integrating these latest technologies, healthcare organizations can improve fraud detection, enhance accuracy, and improve overall financial integrity. The 6 Most Important Developments in Pre-and Post-Payment Audits Advanced Analytics and Artificial Intelligence The integration of advanced analytics and artificial intelligence (AI) technologies has significantly advanced pre-payment and post-payment audits, enabling more accurate identification of potential billing errors, streamlining the audit process, and enhancing overall effectiveness (Huang et al., 2022). In pre-payment audits, AI algorithms analyze large volumes of claims data, identify patterns, and flag anomalies, helping auditors prioritize high-risk claims for review. The use of predictive modeling and machine learning algorithms improves accuracy in identifying potential discrepancies, reducing the burden on auditors. Similarly, in post-payment audits, the application of data analytics and machine learning techniques revolutionizes fraud detection. Advanced algorithms analyze vast amounts of claim data, identifying patterns, anomalies, and potentially fraudulent activities with greater accuracy and speed. This enables auditors to proactively detect and investigate suspicious claims, leading to improved fraud prevention and financial integrity. Real-time Claims Adjudication Real-time claim adjudication systems play a crucial role in both prepayment and post-payment audits. By leveraging these systems, payers can validate claims against billing guidelines and medical policies in real-time, ensuring accurate and compliant payments (Arnold, 2023). In pre-payment audits, the incorporation of automated rule engines and decision support tools allows payers to proactively identify errors or improper billing practices before claims are paid. Real-time adjudication systems provide instant feedback on claim submissions, enhancing provider education and compliance. This immediate validation of claims against guidelines helps prevent payment errors and ensure payment accuracy. Likewise, in post-payment audits, real-time claim adjudication systems help auditors promptly validate claims, detect inconsistencies, and investigate suspicious activities. By providing instant validation and feedback, these systems contribute to improving audit efficiency and effectiveness. Robotic Process Automation (RPA) Robotic Process Automation (RPA) technology has brought significant advancements to both prepayment and post-payment audits. By automating repetitive and rule-based tasks, RPA streamlines the audit process, reduces processing time, and minimizes human errors (Dhanashree, 2022). In pre-payment audits, software robots deployed in RPA assist in tasks such as data entry, verification, cross-referencing multiple data sources, validating provider information, and conducting eligibility checks. These automation capabilities enhance the efficiency and accuracy of pre-payment audits. Similarly, in post-payment audits, RPA technology assists auditors in data validation and verification processes, improving overall audit efficiency. By automating tasks such as data entry and verification, RPA minimizes manual effort, accelerates the audit process, and reduces the likelihood of errors. Machine Learning for Fraud Detection Machine learning techniques have become invaluable for fraud detection in prepayment and post-payment audits. By analyzing claims data using advanced algorithms, machine learning models can identify patterns, anomalies, and potentially fraudulent activities more accurately and quickly (Stiernstedt & Brooks, 2020). In pre-payment audits, machine learning algorithms analyze large amounts of claim data, enabling auditors to identify high-risk claims requiring further review. By proactively detecting discrepancies and potentially fraudulent activities, auditors can improve fraud prevention and ensure financial integrity in the payment process. Similarly, machine learning techniques in post-payment audits revolutionize fraud detection by analyzing claims data for patterns and potentially fraudulent activities. By leveraging these technologies, auditors can proactively detect and investigate suspicious claims, ultimately enhancing fraud prevention efforts and ensuring financial integrity. Predictive Modeling for Risk Assessment Predictive modeling techniques have emerged as valuable risk assessment tools in prepayment and post-payment audits. By analyzing historical claims data, payer-specific patterns, and industry benchmarks, predictive models can assess the risk associated with certain providers, services, or billing practices (Broby, 2022). In pre-payment audits, predictive modeling helps auditors prioritize their efforts by focusing on high-risk areas and optimizing resource allocation for more effective audits. By utilizing predictive modeling, auditors can identify providers or billing practices with a higher likelihood of errors or irregularities, allowing for targeted investigations and improved audit outcomes. Similarly, in post-payment audits, predictive modeling aids auditors in assessing the risk associated with specific providers, services, or billing practices. By analyzing historical claims data and industry benchmarks, predictive models provide insights into potential areas of concern, enabling auditors to allocate their resources efficiently and focus on high-risk targets. This approach enhances the effectiveness of post-payment audits and increases the likelihood of detecting fraudulent activities or billing discrepancies. Blockchain Technology for Audit Trail Transparency Blockchain technology offers enhanced transparency and integrity in both prepayment and post-payment audits by creating an immutable and auditable trail of claims-related transactions. By leveraging blockchain’s decentralized and tamper-proof nature, auditors gain access to a transparent record of claim submissions, payments, and adjustments (Regueiro et al., 2021). In pre-payment audits, blockchain-enabled audit trails ensure the accuracy and reliability of the payment process. Blockchain records’ transparent and immutable nature simplifies the auditing process and provides verifiable evidence, reducing the chances of errors, fraud, or unauthorized modifications. Likewise, in post-payment audits, blockchain technology strengthens the integrity of the audit trail by creating an unalterable record of claims-related transactions. Auditors can rely on blockchain’s transparency and immutability to verify the accuracy of claims, payments, and adjustments, facilitating more efficient and reliable post-payment audits. In Summary Automated workflows and intelligent algorithms streamline the pre and post payment process, optimizing resources and reducing manual errors. Transparent communication with stakeholders, including providers and insurers, resolves discrepancies efficiently and effectively. Regular monitoring and updates adapt to evolving fraud schemes, effectively combating fraud, waste, and abuse. A well-designed payment scrutiny system ensures accurate identification, minimizes errors, and maximizes recovery opportunities. Billing transparency is a top priority at ClinicMind. We are committed to providing you with easy access to comprehensive reporting. With our intuitive system, you no longer have to jump from portal to portal to find answers. We offer over 50 reports that
Fortis: Chiropractic Payment Solutions
In the intricate world of chiropractic practices, where patient care and business operations intersect, finding seamless and efficient payment solutions is paramount. Fortis, a pioneering player in the field of merchant services, has emerged as a game-changer, offering tailored payment solutions designed specifically for chiropractors. In a recent conversation with Jonathan McAleese, CEO of Fortis, we delved into the roots of their journey, the evolution of their services, and the future of chiropractic payment technology. A Legacy Rooted in Chiropractic Care Jonathan’s journey into the world of chiropractic payment solutions is deeply personal. It traces back to his family’s profound connection to chiropractic care, spanning generations. His father’s transformative experience with chiropractic treatment, amidst the challenges faced during his service in the Marine Corps, laid the foundation for Jonathan’s lifelong commitment to the chiropractic profession. With chiropractors woven into the fabric of his family tree, Jonathan’s upbringing immersed him in the world of chiropractic care from an early age. Genesis: A Pioneering Partnership Fortis’ foray into the chiropractic space was catalyzed by a pivotal partnership with Genesis, a leading provider of chiropractic practice management software. Recognizing the unique needs of chiropractors, Fortis Pay integrated seamlessly with Genesis, offering practitioners a comprehensive suite of payment solutions within their existing workflow. From processing credit card payments to managing recurring billing and beyond, Fortis’ integration with Genesis streamlined practice operations, enhancing efficiency and patient experience. Innovative Solutions for Chiropractic Practices Fortis’ commitment to innovation is evident in its relentless pursuit of solutions tailored to the specific needs of chiropractic practices. From simplifying recurring billing to enabling seamless inventory management, Fortis’ offerings are designed to alleviate common pain points faced by chiropractors. The introduction of features like Paylink, allowing for convenient online payments, and forthcoming advancements in inventory management underscore Fortis’ dedication to empowering chiropractors with cutting-edge technology. Looking Ahead: Redefining Chiropractic Payment Technology As Fortis continues to innovate and expand its suite of services, the company remains steadfast in its mission to be a long-term partner to chiropractic practices. Jonathan’s vision for Fortis transcends mere transactional relationships; instead, he envisions a collaborative journey, where Fortis’ technology evolves in tandem with the evolving needs of chiropractors. By staying true to their core principles of reliability, innovation, and customer-centricity, Fortis aims to be the go-to solution for chiropractic payment technology for generations to come. Conclusion In a landscape where technology plays an increasingly pivotal role in healthcare delivery, Fortis stands out as a beacon of innovation and reliability in the realm of chiropractic payment solutions. With a rich legacy steeped in chiropractic care, a commitment to continuous improvement, and a deep understanding of the unique needs of chiropractors, Fortis is poised to revolutionize the way chiropractic practices manage their payments. As chiropractors navigate the complexities of running their practices, Fortis Pay remains a trusted partner, empowering them to focus on what matters most: delivering exceptional care to their patients. Genesis Nation, take note: the future of chiropractic payment technology is here, and it’s powered by Fortis.
Straight-Through Billing

Medical billing complexity and massive volumes of daily claims render manual claims processes incapable of protecting both the provider and the payer from underpayments, overpayments, and billing compliance violations. Straight-Through Billing (STB) addresses complexity and volume processing problems by automating the majority of the claim flow and focusing the billing follow-up specialists on exceptions only. An STB process flags problems routes them for follow-up and enables online correction and resubmission. The STB methodology implements billing service transparency and focuses management on strategic process improvement opportunities. Straight-Through Billing integrates the billing process into the practice management workflow, automates the vast majority of transactions, focuses manual labor on exceptions, and establishes a process for continuous improvement. Remember: Straight-Through Billing offers a comprehensive approach to improving the billing process, integrating various components, and promoting continuous improvement. Practice Management Integration First, integrated practice management and billing workflow connects patient scheduling, medical record management, and billing into a single process. Every participant in the practice management workflow receives a unified and coherent picture of the practice workload, patient and provider location, resource availability, and cash flow. However, integrated with Electronic Health Records, practice management systems are more beneficial. Electronic health records (EHR) are digital formats of a patient’s chart. They contain all the information about a patient’s health. This includes medical history, allergies, immunizations, previous treatments, medication history, past diagnoses, history of substance abuse (if any), and so forth (Shah, 2021). Transaction Automation Transaction automation streamlines and expedites the billing process by automating claim validation, payer message reconciliation, and billing workflow management: Automated claim validation eliminates errors downstream and reduces processing time because it flags errors before submitting the claim to the payer. Automated claim message reconciliation eliminates the costly search for the original claim and standardizes message communication, eliminating the need to decipher the (often cryptic) payer’s message. Automated billing workflow management drives the follow-up discipline required for the resolution of claim denial and underpayment incidents, and it establishes a high degree of process transparency for all billing process participants, resulting in full and timely payments. Automated billing increases the net collection rate due to quick claim turnaround and efficient follow-up. Respond to your denials within 5-21 business days of receiving them, using our Daily Denial Email Alerts (Qureshi, 2022). Focus on Exceptions Focusing manual labor on exceptions requires timely exception identification, routing to follow-up personnel, online error correction, and rigorous follow-up tracking. Again, process transparency enables tracking exception follow-up as implemented in ClinicMind-like systems. Another significant benefit of automated medical billing is the ability to track and analyze financial data. With this, healthcare facilities can monitor their revenue cycles, identify growth opportunities, and generate detailed financial reports (Polo, 2023). Continuous Process Improvement Finally, a process for continuous improvement requires continuous observability of every process attribute and a modification methodology for both automated claim processing and manual exception follow-up tracking. Straight-Through Billing implements billing transparency by design because billing transparency is an integral attribute of every component of the STB process. It also enables businesses to streamline their billing operations, reduce errors, enhance efficiencies, and improve the customer experience (Ward, 2023). Straight-Through Billing Architecture The Straight-Through Billing systems architecture mirrors the architecture of general Straight-Through Processing (STP) systems developed for the financial services industry. Such systems require effective workflow management, a knowledge-based validation system, connectivity to all process participants (including online data reconciliation), and tracking of problem resolution. Therefore, a typical ClinicMind-like STB system has a three-tiered architecture: Back-end processing engine designed for a high-volume transaction processing environment Middle tier, using Java Servlet technology Front end, using an HTML-JavaScript, zero-footprint client Did You Know? The STB architecture is inspired by the systems used in the financial services industry, showcasing the transferability of advanced processing concepts across different domains. An STB system (e.g., ClinicMind) based on the methodology outlined here implements rich functionality, which allows the following to be automated: Computer-aided preferential patient scheduling Integrated electronic medical records Online computer-aided coding Real-time claim validation and patient eligibility testing Electronic claim submission Payment posting, reconciliation, and verification of meeting contractual obligations Monitoring of audit risk and billing compliance Tracking of denial appeal process Quantitative STB Management Straight-Through Billing methodology allows for quantitative management since the likelihood of the entire process failing can be estimated as the product of such items for each individual workflow step. A ClinicMind-like STB system tracks the percentage of clean claims (claims paid in full, and within the allocated time frame, without any manual intervention) and focuses the management on those process aspects that yield the greatest potential improvement. Thus, STB methodology focuses on exceptions at both the tactical and strategic management levels and can help to improve cash flow and reduce outstanding invoices by providing real-time visibility into billing and payment status (Mielnicki, 2022). Modern Insights and Research In the ever-evolving field of medical billing, staying ahead of the curve is crucial for achieving financial excellence in the healthcare industry. Let’s embark on an exhilarating journey into the future of medical billing, where the convergence of electronic health records (EHRs), artificial intelligence (AI), real-time analytics, and collaborative efforts reshapes the revenue cycle landscape. Brace yourself for a transformative exploration that revolutionizes processes, enhances data accuracy, maximizes financial outcomes, and ushers in an era of unparalleled efficiency and effectiveness in the dynamic realm of medical billing. 1- Role of Blockchain Technology in Billing Systems The seamless integration of electronic health records (EHRs) and billing systems is revolutionizing the field of medical billing. Gone are the days of fragmented medical records scattered across various healthcare organizations. With blockchain at the helm, a distributed EHR ecosystem emerges, ensuring a smooth flow of information between providers. By eliminating manual data entry and ensuring accurate documentation, this innovative technology guarantees accurate and secure documentation, eliminating errors and speeding up reimbursement processes (Cerchione et al., 2022). But that’s not all. Blockchain brings an unparalleled level of data integrity and security, employing cryptographic techniques to safeguard patient information from prying eyes.
Decoding the Complexities of Chiropractic Billing and Coding
With over 16 years of chiropractic practice, Dr. Marty Kotlar from Target Coding brings a unique blend of real-life experience and coding expertise, holding certifications as a Professional Compliance Officer and Billing and Coding Specialist. In this conversation with Genesis, Dr. Kotlar shares his insights and sheds light on the top three mistakes chiropractors commonly make in billing, coding, and compliance. Insurance Practices Dr. Kotlar kicks off our discussion by emphasizing the importance of meticulous tracking in insurance-based practices. He introduces the concept of an insurance tracking spreadsheet, stressing the need to record every payment accurately to avoid potential discrepancies. He also touches on common issues such as copay discrepancies and claim processing errors, urging practitioners to ensure they receive rightful reimbursement. Moving on, Dr. Kotlar delves into the world of codes. He discusses the nuances of time-based codes and non-time-based codes, providing valuable insights into maximizing reimbursement through proper coding. Exploring the intricacies of time-based codes like therapeutic exercises (97110), he unveils the critical factors providers should consider for accurate coding. In the final segment of insurance practices, Dr. Kotlar addresses the challenge of maximizing reimbursement. He shares pearls of wisdom, including the often-overlooked activities of daily living (ADLs) code (97535) and the significance of extremity adjustments. By unraveling the complexity of re-exams and other reimbursable services, Dr. Kotlar provides actionable strategies for practitioners aiming to optimize their revenue in insurance-based practices. Personal Injury (PII) Shifting the focus to personal injury (PII) practices, Dr. Kotlar enlightens us on the crucial role SOAP notes play in building strong cases for attorneys. He emphasizes the importance of documenting “duties under duress” and “loss of enjoyment of life,” elements that can significantly impact the patient’s life post-accident. Dr. Kotlar discusses the potential pitfalls associated with overprescribing in PII cases, cautioning against unnecessary procedures or devices. He sheds light on compliance challenges related to devices like back braces, TENS machines, and home traction units. Additionally, he underscores the necessity of thorough follow-ups to prove the clinical necessity of prescribed items. In this segment, Dr. Kotlar unveils the complexities of fee schedules, dual fee schedules, and the state-specific regulations chiropractors must navigate in the PII landscape. By addressing these challenges, he equips practitioners with the knowledge needed to build strong PII practices while ensuring compliance with legal and ethical standards. Cash Practices Dr. Kotlar concludes our conversation by exploring the nuances of cash practices. He starts by cautioning against misleading advertising practices, emphasizing the need for compliance even in cash-based settings. The discussion then pivots to the intricacies of prepaid plans, highlighting the potential risks associated with mishandling prepaid funds and the necessity of putting money in escrow. The conversation takes an insightful turn as Dr. Kotlar delves into the complex realm of discounts in cash practices. He demystifies the restrictions and allowances surrounding discounts, providing practitioners with a clearer understanding of how to navigate this aspect successfully. The final focus of our discussion centers on distinguishing between medically necessary care and maintenance or wellness care in cash practices. Dr. Kotlar outlines the importance of accurately coding services based on the nature of the patient’s visit, offering practical guidance for maintaining compliance and avoiding pitfalls. Conclusion: As our enlightening conversation with Dr. Marty Kotlar concludes, chiropractors and practitioners in allied fields gain a wealth of knowledge to enhance their billing and coding practices. Dr. Kotlar’s expertise and insights serve as a compass, guiding practitioners through the intricate landscape of compliance, reimbursement optimization, and ethical considerations. In the ever-evolving field of chiropractic care, staying informed and proactive is key, and Dr. Kotlar’s wisdom provides a valuable roadmap for success. Stay tuned for Part 2 of this conversation to be released next week! Experience the entire episode by viewing it through: https://bit.ly/3U5sACL

